As the country nears the “end of the beginning” of the COVID-19 crisis, healthcare organizations are struggling to understand how to pivot from containment to recovery. As the industry continues to gain knowledge regarding risks, signs, symptoms, testing, and treatment of COVID-19, we have found ourselves amidst an astronomical shift in priorities, best practices, and future planning.
What can we do with the deluge of varying recommendations, limited COVID-19 claims data, and unknown impact we have in front of us today? For health plans, identifying and monitoring high-risk comorbid member populations, tracking the shift to telehealth utilization, and evaluating the short- and long-term financial impacts are three steps that could help them achieve the Triple Aim in this challenging environment—and better prepare and strategize for a potential second wave of the virus.
Here are three key concerns payers will need to address as they work through these steps.
Understand risk and cost drivers and inform disease management strategies
The coronavirus outbreak is challenging payers and providers to manage not only an influx of patients with a new and poorly understood disease, but also those with existing complex, chronic diseases such as diabetes, heart disease, and addiction. For many, managing these chronic diseases has taken a backseat: members are avoiding doctor visits for acute problems, and have had well visits and routine care delayed or canceled as providers work to contain and prevent the spread of COVID-19. At the same time, there is emerging evidence that COVID-19 could have long-lasting effects for certain patients, well after they recover from the acute phase. Chief among these are negative effects on the heart, kidneys, and brains from impaired lung function. Front-line healthcare workers and their families are at increased risk for post-traumatic stress disorder, anxiety, depression, and substance abuse.
Moving forward, to prepare and allocate resources for disease management strategies, health plan decision-makers must revisit their strategies for managing known, existing conditions while working to gain a new understanding of the prevalence of vulnerable, high-risk comorbid conditions of COVID-19 in their member population. They can start by answering the following questions:
- Which high-risk conditions are most prevalent?
- What percentage of the high-risk population has been diagnosed with COVID-19?
- What is the cost and future risk of these populations?
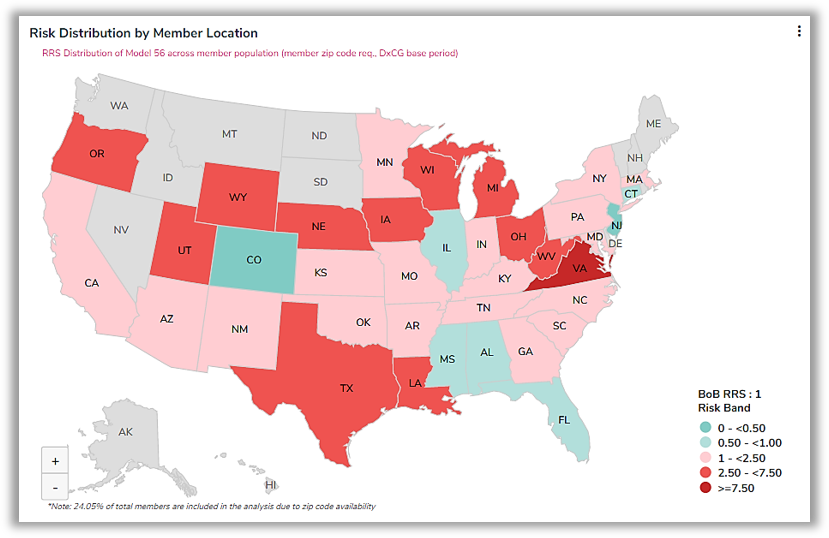
- Where are the most high-risk patients located?
Figure 1: Risk distribution by member location, shows how DxCG data can be used to identify risk severity by state and the volume of your population with highest risk or populations diagnosed with COVID-19 or at-risk COVID-19 groups. This data can also drill down to the county level and respective list of members.
Evaluate utilization shifts
Even before the COVID-19 pandemic, federal and state governments were enacting significant policy changes to encourage more widespread use of telehealth options. Now, necessary social distancing and patient safety regulations have pushed telehealth to the forefront as a promising tool in maintaining the continuity of care for chronic conditions.
Moving forward, designing a strong telehealth strategy will be key to keeping members with chronic conditions healthy and engaged. In designing such a strategy, health plans must capture and account for the shift of various types of healthcare utilization to telehealth. To fully understand opportunities and challenges in increasing telehealth access, health plans should start their investigations by gathering this data:
- How has the shift to telehealth impacted other utilization trends and associated cost?
- Who is using telehealth and what conditions do they have?
- What is the impact to gaps in care compliance rates?
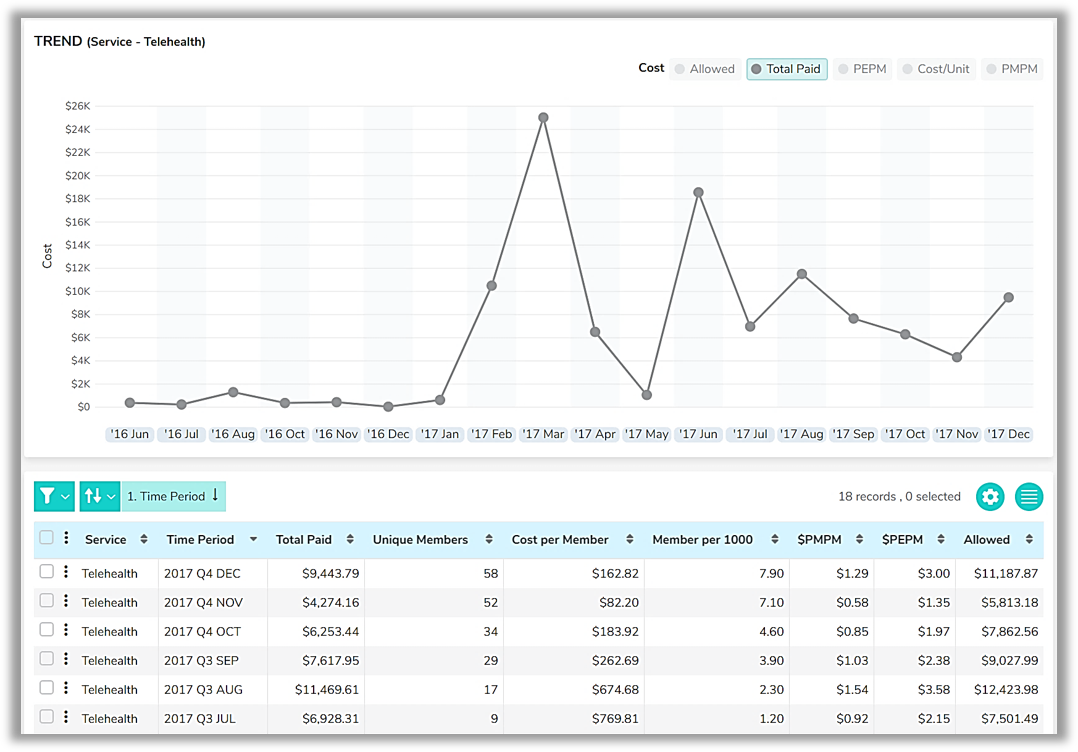
Figure 2: Telehealth trends, highlights data that can help plans better understand the costs and diagnoses associated with telehealth utilization.
Understand impacts to population health outcomes
Although it’s clear that the acute phase of the COVID-19 crisis will continue for some time, it’s not too soon to plan for the longer-term impacts to population health and changes in membership makeup. The stress and isolation created by the pandemic and subsequent stay-at-home and social distancing measures is already manifesting itself in myriad behavioral health and addiction problems, in addition to a possible rise in domestic abuse. Delayed care for both chronic health issues and elective procedures will carry significant health and financial impacts. Furthermore, understanding the prevalence of vulnerable, high-risk comorbid conditions of COVID-19 in membership populations will help health plan leaders make informed decisions as they prepare and allocate resources for ongoing disease management strategies.
Massive layoffs caused by the shutdowns will change the face of a health plan’s membership rolls, not only with attrition in commercial plans and increased membership in Medicare and Medicaid plans, but also with substantial changes in health and risk mix in all plans. To get a handle on what could lie ahead in the coming months, health plans should ask:
- What is the impact to the behavioral health population?
- Has behavioral health prevalence increased in the last three months?
- How has the inpatient utilization trend been impacted by behavioral health?
- What are the critical and/or actionable diagnoses of behavioral health in the population?
- What is the impact on delayed care (e.g., elective surgeries and procedures)?
- What providers and specialties have a rapid increase of elective procedures?
- What conditions are associated with the most recent spike in elective procedures?
- What is the highest paid/most prevalent elective procedure in most recent months?
- What procedures were still occurring during the pandemic vs procedures with complete gaps in trend?
- What is the rate of termed members month over month?
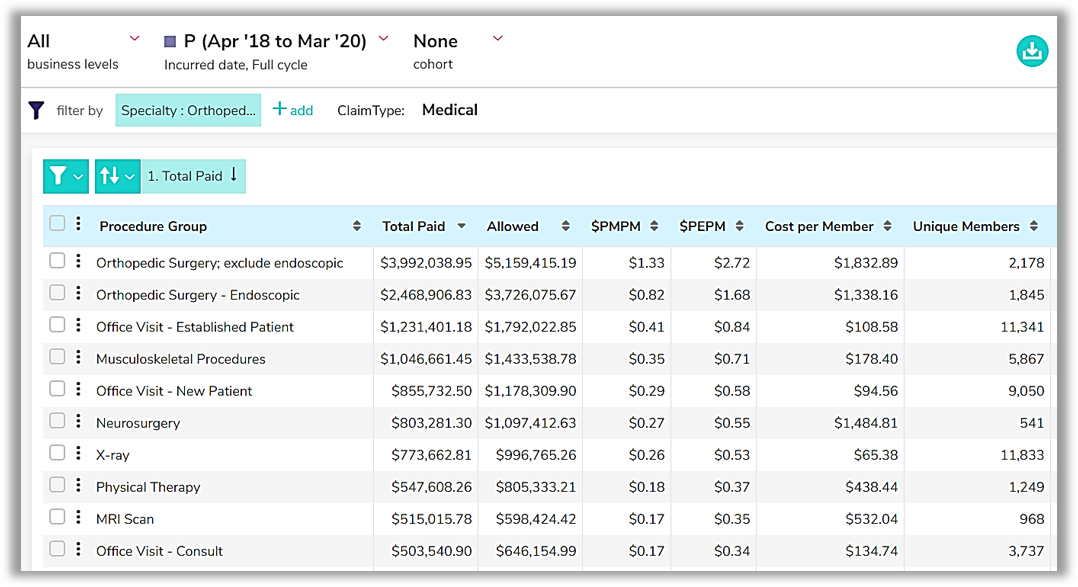
Figure 3: Elective procedure claims, shows data that allows plans to analyze elective procedure groups by provider or specialty to understand areas with the greatest impact.
By leveraging insights gained through advanced data analytics, health plans can start to develop short and long-term strategies to support the health and safety of their ecosystem by understanding what puts their populations at risk, closely tracking the incoming COVID-19 data, and planning for anticipated impacts.
To succeed in managing population-based clinical and financial risk, payer organizations need answers to highly complex questions about healthcare costs, quality, and utilization. Download our fact sheet to learn how Medical Intelligence combines Cotiviti’s industry-leading DxCG science with evidence-based clinical quality rules, healthcare utilization metrics, and claims-based HEDIS® measures to enable payers to manage risk and target opportunities for improving healthcare results.
HEDIS® is a registered trademark of the National Committee for Quality Assurance (NCQA).



